Expo
view channel
view channel
view channel
view channel
Medical Imaging
AI
Surgical TechniquesPatient CareHealth ITPoint of CareBusiness
Events
Webinars

- Cancer-Seeking Microbubbles Make Tumor Cells Self-Destruct
- Eye Movement Tests Uncover Hidden Brain Changes Years After Concussion
- Simple 5-Minute Questionnaire Test Speeds Endometriosis Diagnosis
- Nanohydrogels Guide Medicine to Tumors Without Damaging Healthy Tissue
- Magnetic Gel Offers Safer and More Effective Atrial Fibrillation Treatment
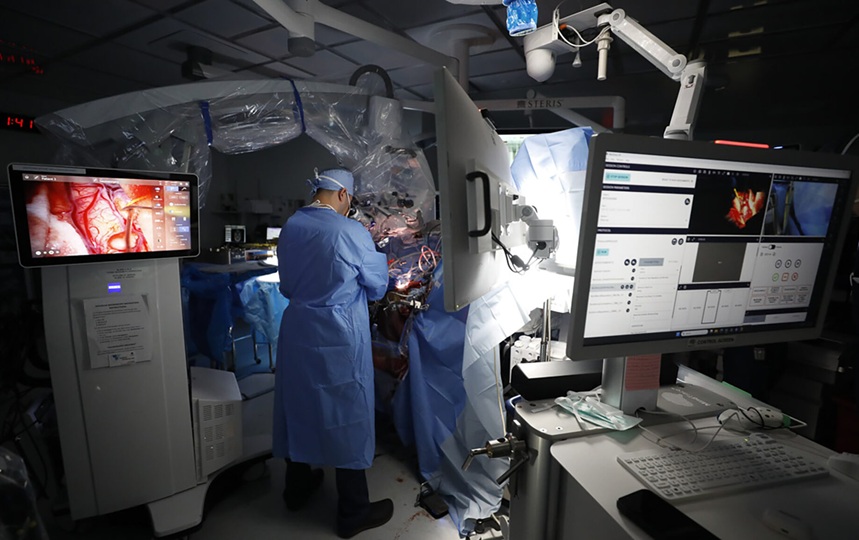
- Robot-Assisted Brain Angiography Improves Procedural Outcomes
- Brain Mapping Technology Enhances Precision in Brain Tumor Resection
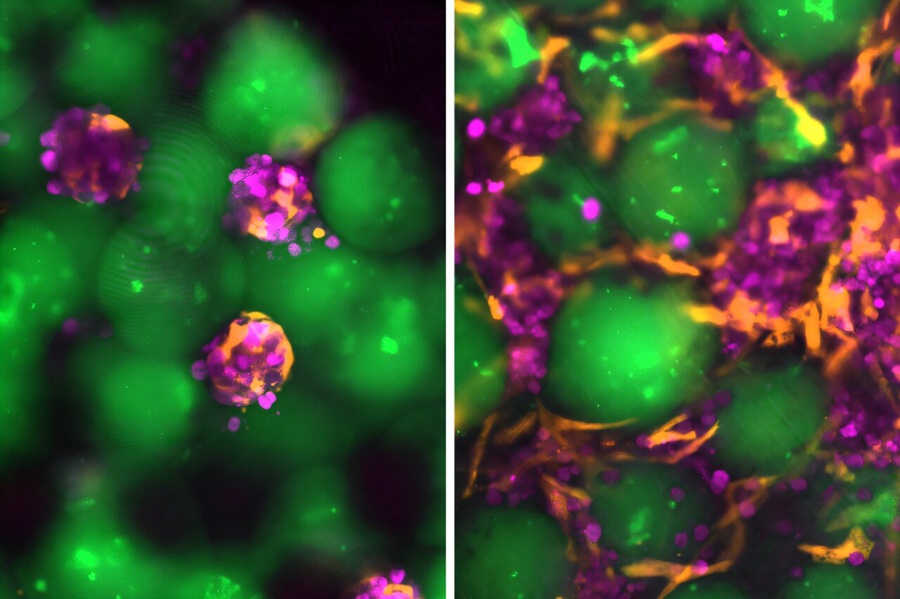
- Injectable Mini Livers Offer Hope for Patients Awaiting Transplant
- Pulsed Field Ablation Technology Cleared in Europe for Persistent AFib
- AI-Powered Imaging Brings Real-Time Margin Clarity to Breast Cancer Surgery
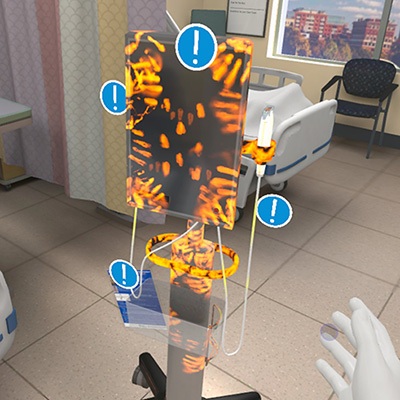
- VR Training Tool Combats Contamination of Portable Medical Equipment
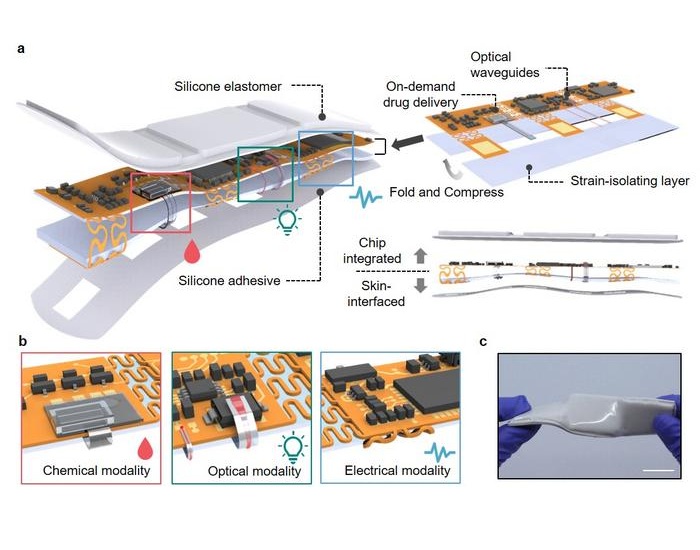
- Portable Biosensor Platform to Reduce Hospital-Acquired Infections
- First-Of-Its-Kind Portable Germicidal Light Technology Disinfects High-Touch Clinical Surfaces in Seconds
- Surgical Capacity Optimization Solution Helps Hospitals Boost OR Utilization
- Game-Changing Innovation in Surgical Instrument Sterilization Significantly Improves OR Throughput
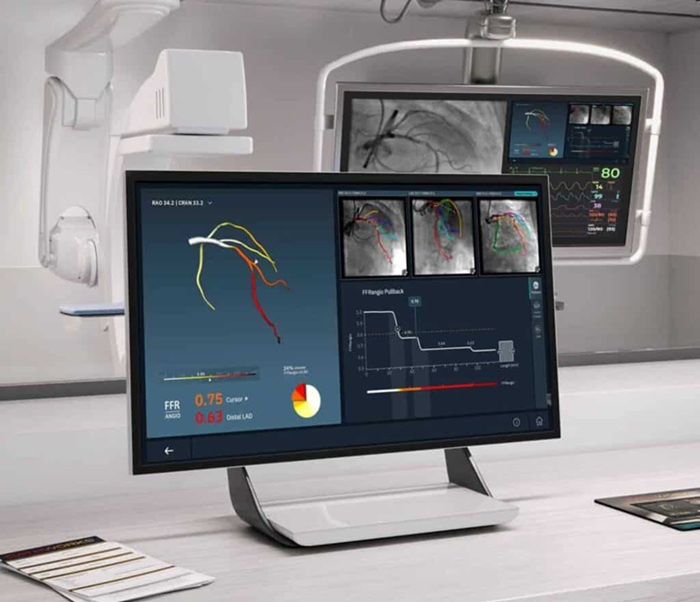
- Medtronic to Acquire Coronary Artery Medtech Company CathWorks
- Medtronic and Mindray Expand Strategic Partnership to Ambulatory Surgery Centers in the U.S.
- FDA Clearance Expands Robotic Options for Minimally Invasive Heart Surgery
- WHX in Dubai (formerly Arab Health) to debut specialised Biotech & Life Sciences Zone as sector growth accelerates globally
- WHX in Dubai (formerly Arab Health) to bring together key UAE government entities during the groundbreaking 2026 edition

 Expo
Expo
- Cancer-Seeking Microbubbles Make Tumor Cells Self-Destruct
- Eye Movement Tests Uncover Hidden Brain Changes Years After Concussion
- Simple 5-Minute Questionnaire Test Speeds Endometriosis Diagnosis
- Nanohydrogels Guide Medicine to Tumors Without Damaging Healthy Tissue
- Magnetic Gel Offers Safer and More Effective Atrial Fibrillation Treatment
- Robot-Assisted Brain Angiography Improves Procedural Outcomes
- Brain Mapping Technology Enhances Precision in Brain Tumor Resection
- Injectable Mini Livers Offer Hope for Patients Awaiting Transplant
- Pulsed Field Ablation Technology Cleared in Europe for Persistent AFib
- AI-Powered Imaging Brings Real-Time Margin Clarity to Breast Cancer Surgery
- VR Training Tool Combats Contamination of Portable Medical Equipment
- Portable Biosensor Platform to Reduce Hospital-Acquired Infections
- First-Of-Its-Kind Portable Germicidal Light Technology Disinfects High-Touch Clinical Surfaces in Seconds
- Surgical Capacity Optimization Solution Helps Hospitals Boost OR Utilization
- Game-Changing Innovation in Surgical Instrument Sterilization Significantly Improves OR Throughput
- Medtronic to Acquire Coronary Artery Medtech Company CathWorks
- Medtronic and Mindray Expand Strategic Partnership to Ambulatory Surgery Centers in the U.S.
- FDA Clearance Expands Robotic Options for Minimally Invasive Heart Surgery
- WHX in Dubai (formerly Arab Health) to debut specialised Biotech & Life Sciences Zone as sector growth accelerates globally
- WHX in Dubai (formerly Arab Health) to bring together key UAE government entities during the groundbreaking 2026 edition















.jpg)